cointosser13
Forum Crew Member
- 63
- 4
- 8
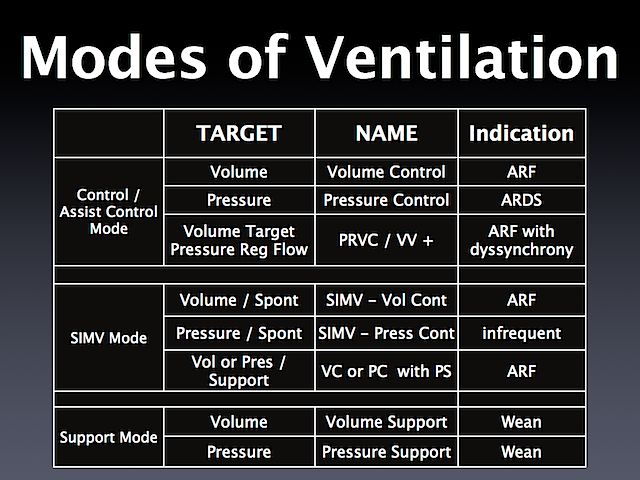
This more pertains to critical care paramedicine, but I was wondering: how do you remember what each vent mode (A/C PRVC SIMV etc) does when ventilating a patient? Any tricks (or charts) to remembering what each one does?