I'm gonna throw in a call we had. Interesting stuff happened.
You are a CCT crew called code 3 to a hospital's telemetry floor for an urgent STEMI transfer to a hospital with a cath lab. Your transport time will be 11min from hospital to hospital and you have 1 CCT-RN and 2 EMT's on board.
You arrive on scene to find 6 RN's and a crash cart next to the room of an elderly male patient, AX0X4 but appears very weak lying supine with the following vitals: HR118, BP 69/49, R8 labored, SP02 77% on 6L NC. PmHx: Hyperlipidemia, hypertension. No current meds, no current allergies. A 1L NS bolus is running wide open, no additional meds have been ordered.
The patient's primary RN states that the patient is DNR/DNI. The staff says that the patient was admitted for stomach pain 2 days prior and diagnosed him with new onset gallstones. He developed sudden chest pressure in the AM and when a 12 lead was sent to the hospitalist, he arranged transfer for his diagnosis of a STEMI.
At this point, the CCT-RN asks the patient to confirm his DNR status given the situation and the patient now says he wants everything to be done to save his life, so his status was changed to a full code.
The patient is raised to semi-fowlers from supine and a 15L NRB is applied in addition to the 6L NC already on. SP02 raises to 87%, R10 but still labored. The patient now says that he needs some suction to help him spit and you notice bright red blood, approximately a handful's worth.
One of your EMT's is helping suction the patient and keep him calm while the other is hooking him up to the Zoll transport monitor.
CCT-RN begins asking for pressors. What pressors/medications would you ask for since only NS is running? Would you ask for an MD or and additional RN to come along with you on this call as well?
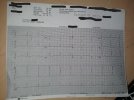
12 lead from the hospital is attached as well as the rhythm strip from the transport monitor. Be advised, there was a 3hr delay from when the 12lead was taken/sent to the Dr and when urgent transfer was arranged.
More to come...
You are a CCT crew called code 3 to a hospital's telemetry floor for an urgent STEMI transfer to a hospital with a cath lab. Your transport time will be 11min from hospital to hospital and you have 1 CCT-RN and 2 EMT's on board.
You arrive on scene to find 6 RN's and a crash cart next to the room of an elderly male patient, AX0X4 but appears very weak lying supine with the following vitals: HR118, BP 69/49, R8 labored, SP02 77% on 6L NC. PmHx: Hyperlipidemia, hypertension. No current meds, no current allergies. A 1L NS bolus is running wide open, no additional meds have been ordered.
The patient's primary RN states that the patient is DNR/DNI. The staff says that the patient was admitted for stomach pain 2 days prior and diagnosed him with new onset gallstones. He developed sudden chest pressure in the AM and when a 12 lead was sent to the hospitalist, he arranged transfer for his diagnosis of a STEMI.
At this point, the CCT-RN asks the patient to confirm his DNR status given the situation and the patient now says he wants everything to be done to save his life, so his status was changed to a full code.
The patient is raised to semi-fowlers from supine and a 15L NRB is applied in addition to the 6L NC already on. SP02 raises to 87%, R10 but still labored. The patient now says that he needs some suction to help him spit and you notice bright red blood, approximately a handful's worth.
One of your EMT's is helping suction the patient and keep him calm while the other is hooking him up to the Zoll transport monitor.
CCT-RN begins asking for pressors. What pressors/medications would you ask for since only NS is running? Would you ask for an MD or and additional RN to come along with you on this call as well?
12 lead from the hospital is attached as well as the rhythm strip from the transport monitor. Be advised, there was a 3hr delay from when the 12lead was taken/sent to the Dr and when urgent transfer was arranged.
More to come...